What is Pericoronitis?
There are various problems associated with dental and oral health. One of the most frequent one is pericoronitis.
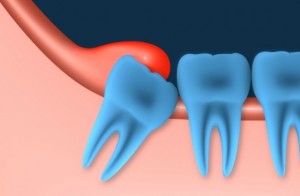
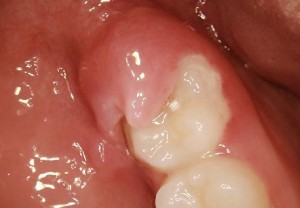
Pericoronitis can develop when a tooth only partially erupts. It is a disorder in which the gum tissue around an incompletely erupted tooth (crown portion) becomes swollen and infected. This disorder usually occurs as a result of 3rd molar or wisdom tooth where gum tissue overlaps the chewing surface of the tooth.
The third and final set of molars most people get in their teens or early twenties. The wisdom teeth that are usually affected are the ones in the lower jaw.
When a person’s wisdom tooth just start to protrude through the gums, it allows an opening for bacteria to enter around the tooth as it creates a flap of gum tissue that easily holds food particles and debris after eating. As the hygiene of the area is not very easy to maintain, the presence of food waste can be constant and plaque bacteria will grow, causing inflammation and infection in the area.
This gum flap is a hotbed for germs which results in infection. If it remains there, it can irritate the gum and lead to pericoronitis. If the pericoronitis is severe, the swelling and infection may extend beyond the jaw to the cheeks and neck.
Pericoronitis can be either chronic or acute. Chronic pericoronitis is a mild persistent inflammation of the area. Acute pericoronitis is when the symptoms intensify to fever, swelling, and pain, which indicate a spreading infection.
Pericoronitis is differentiated from gum disease (or periodontitis) in that it occurs specifically around a partially erupted tooth where the tooth has not completely emerged from the gum overlying it. The cause of this condition is similar to the formation of a gum abscess in periodontitis by the entrapment of debris under the gum tissue.
Getting pericoronitis is one of the main reasons that you have your wisdom teeth extracted.
Complications can occur with pericoronitis. Although rare, the infection can spread from the mouth into the head and neck and cause a serious complication called “Ludwig’s angina.” This can be a life-threatening condition where the airway could be blocked. Another life-threatening concern is the spread of the infection to the bloodstream (sepsis).
With timely care and treatment, pericoronitis can properly be managed or eliminated. Infact dental clinics in Delhi like ours ie ‘Smile Delhi-The Dental Clinic’ are making it a norm to remind their patients to come for a six monthly check and clean, as these problems remain silent for a long time.
What causes pericoronitis?
The primary cause for pericoronitis is accumulation of bacteria. Usually, the tooth is only partially exposed (erupted) and has excess gum tissue that overlaps the tooth. Bacteria and food debris gets trapped in the space between the tooth and the overlapping gum.
Active infection is associated with an abscess that contains pus, which has the ability to spread if left unattended.
Bad hygiene in that area
Stress and fatigue
Mensturation
Second trimester of pregnancy
Other mouth and throat infections
What are pericoronitis symptoms and signs?
Signs and symptoms of pericoronitis can range from mild to severe pain. In the area of the affected tooth, the gum tissue is swollen and red, bad breath can be caused by bacteria and food trapped under the gum flap, bad taste in the mouth caused by pus leaking from the gums, difficulty opening the mouth due to stiffness in the jaw because the swelling/inflammation has spread to affect the muscles that move your jaw.
In more severe cases, symptoms may also include fever, difficulty in swallowing, swelling of the lymph nodes in the neck, sore throat, earache, loss of appetite, and feeling unwell.
Moreover, as this area will be swollen, it is quite possible that the opposite tooth above the area exacerbates the problem by biting down on the swollen gum causing more swelling and pain.
If your tooth, jaw, and cheek are swollen and painful, see your dentist right away.
What is the treatment for pericoronitis?
The treatment will depend on the severity of the disease and the symptoms that you are present with, but essentially the aim is to treat the infection and remove the cause.
One thing that you should not do is apply heat to the area as it can promote the spread of the infection toward the skin on your face.
Dental clinics in India are routinely treating pericoronitis by various treatment methods. There are three methods for treatment of pericoronitis depending on the severity of the condition.
1. Management of pain and resolving the infection if the pericoronitis is limited to the tooth (for example, if the pain and swelling has not spread)
- Improving oral hygiene to keep the area cleaner.
- Rinsing with warm salt water frequently and cleaning the area thoroughly. You should also make sure that the gum flap has no food trapped under it.
- Rub an ice cube rolled up in a towel gently over the cheek near the site of impacted tooth for about 5min.
- To avoid irritating your gum tissue you should eat a soft diet. For the infection the dentist may prescribe medications such as antibiotics and pain relievers.
2. Minor surgery to remove the overlapping gum tissue
When the tooth can be useful and there is a desire to keep the tooth, minor surgery can be performed to remove the gum tissue covering the tooth portion. This will allow better access to properly clean the area and prevent the accumulation of bacteria and food debris. In some unfortunate instances, the gum tissue may grow back and create the same problem.
3. Removal of the tooth
If the pain and inflammation are severe, or if the pericoronitis recurs, or if the tooth is never likely to be useful, for example, because the top wisdom tooth has been removed, or it is impacted and trapping , generally it would be better off removed (assuming there is not a high risk of complication). Removal (extraction) of the tooth under local anaesthetic is the most common treatment method since wisdom teeth often times are poorly positioned and do not erupt completely. This method eliminates any future occurrences of pericoronitis.
It is a matter of weighing up the benefits of removing wisdom teeth versus the risks of having it out.
Usually pericoronitis symptoms can be relieved with the treatment in about seven days. It will most likely return if the bacteria and food debris keep building up under the gum and the tooth is still partially impacted and not removed.
It is necessary to intensify the cleaning of the area, in order to remove food particles and plaque bacteria that have accumulated below the gum. Dentists in Delhi regularly counsel patients to do warm salt water rinses at least four times throughout the day to help settle the inflammation of the gums.
In the vast majority of cases, this condition is managed routinely with your dentist. Untreated pericoronitis can be very painful and in severe cases dangerous as the area is very close to the airway in the neck and lead to infection in the neck.
Swelling in this area could cause difficulty breathing and swelling in the neck puts you at considerable risk, requiring hospital admission and to be treated with intravenous antibiotics.
Is it possible to prevent pericoronitis?
Prevention of pericoronitis may be achieved with regular dental visits and preemptive care. The dentist can aid in keeping these potential problem areas clean. Dentists in India monitor the eruption of the third molars and determine the need for early extraction of these teeth. Removal of the wisdom teeth prior to eruption can prevent pericoronitis.
Posted By – Dr. Shriya