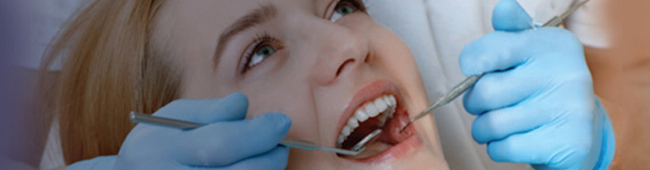
Occupational Hazards To Dentists and Dental Staff
Dentists and other health care workers have long been concerned about a variety of infectious agents that may be transmitted within the dental setting.
Dental professionals are predisposed to a number of occupational hazards.
The oral cavity is a natural habitat for a large number of microorganisms. This is of particular importance in the case of routine dental practice, as the risk of exposure to microorganisms in the oral cavity is increased due to the open and invasive nature of the procedures.
These include exposure to blood borne or air borne pathogens like Human Immunodeficiency Virus and viral hepatitis and tuberculosis etc.
There are a number of possible means by which transmission of viral and bacterial pathogens can occur in the dental practice. The patient’s own saliva and blood are major vectors of cross-transmission.
Blood-borne contamination can occur by exposure to the infectious material through non-intact skin and mucosal lesions.
Dental clinic in Delhi are routinely counseling patients that they may be at increased risk for complications from certain diseases if they have a chronic health condition or weakened immune system but they could be prevented by vaccines.
The highest infectious risk of this type is associated with accidental punctures by contaminated needles or injuries by sharp instruments.
Because of the increased potential for exposure to bodily fluids, dental professionals carry specific risks for disease transmission.
In some cases, diseases can remain latent in a person for years and become activated when the immune system is vulnerable (such as with tuberculosis and herpes zoster).
Most exposures to infectious microorganisms do not result in the transmission of infectious diseases partly because a person’s vaccinations and immune system protect against contracting illnesses.
In addition, not all diseases are equally virulent, and the frequency and degree of exposure also play a role in whether a person contracts an infection.
It is a good policy to postpone elective treatment during the infective period which improves the patient’s comfort and eliminates the risk of infection.
Much attention has been focused on convalescent and asymptomatic carriers of infection as these patients are often infective and the infections represent some of the most serious risks of transmission in the dental practice and the carriers cannot be readily identified.
Those patients who carry hepatitis B virus (HBV) and hepatitis C virus (HCV) cannot be identified, but a good medical history is useful since some people will know their carrier status.
Dentists in India are keeping themselves immunized with the help of vaccinations so that they can treat such patients.
Some of the most common infectious diseases that are concern to dental healthcare providers are-
Herpes viruses
Cross-transmission risks in dentistry are mainly related to herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2) and to varicella-zoster virus (VZV).
Oral secreta can also be infectious and constitute a risk of cross-transmission.
HSV is highly contagious and is transmitted via exposure of the mucosa or skin to infectious secreta or contents of an infectious HSV blister.
Unless adequate personal protection is worn, the dental team and the patient are at risk of being exposed to HSV via direct contact with herpetic ulcers or infectious splatters from herpetic lesions or saliva.
HSV is very infectious and patients commonly attend dental clinic with a herpes labialis or cold sore which can infect the dentists.
This could result in mucosal or skin infections, keratitis or herpetic whitlows which are intensely painful lesions. Outside the body HSV is inactivated within hours and is easily inactivated by disinfectants, such as alcohols.
The frequency of herpetic whitlow was observed to be higher among practicing dentists compared to the normal population
Chickenpox is the manifestation of VZV primary infection. VZV can be also asymptomatically shed in saliva. Immune suppressed patients are at increased risk for disseminated disease and in non-immune pregnant women fetal infections are possible.
VZV is a highly contagious virus. It is transmitted through direct contact to the blisters or exposure to infectious droplets from saliva or the respiratory system. Airborne transmission is also possible.
VZV infection constitutes a risk for healthcare-associated transmission of VZV in the dental practice as well.
Hepatitis B virus
Hepatitis B virus is a real threat for cross-infection in dentistry.
Hepatitis B is a blood-borne and sexually transmitted virus, which causes inflammation of the liver.
The hepatitis B virus (HBV) may be transmitted through contact with bodily fluids from a person with either an active or chronic HBV infection. It has high level of viral replication and increased infectivity.
HBV infection can result from having unprotected sex with an infected individual, by an infected mother to her infant at birth, percutaneous injuries (in) direct blood or body fluid exposure through open sores of an infected person such as scratches, abrasions, burns or on mucosal surfaces, through needle sticks and other contaminated exposures and by sharing household items such as razors and toothbrushes with an infected person.
HBV has demonstrated the ability to survive and remain infectious in dried blood outside the body at room temperature on environmental surfaces for at least 1 week and probably longer
Vaccination of healthcare workers for HBV has greatly reduced the risk of transmission of HBV. However, HBV is highly infectious and even after the vaccine became available, healthcare providers remained at risk for HBV infection.
The risk of transmission of HBV through the dental practice remains an issue.
The use of proper disinfection and sterilization procedures and appropriate personal protective attire is important for preventing the transmission of HBV in the dental office setting.
Hepatitis C virus
Hepatitis C virus (HCV) infection is the most common chronic bloodborne infection.
Chronic infection means that the virus is actively replicating in the liver and circulates in the blood and other bodily fluids.
Infected individuals may transmit HCV. The most common means of transmission is through illegal-injection drug use.
Other means of transmission include blood and blood product transfusions and organ transplantation.
Rarely, HCV may be transmitted sexually or by sharing personal items contaminated with blood. Sharps injuries in healthcare have also resulted in HCV transmission, although transmission via this route is less likely than it is with HBV.
Infants born to infected mothers may also contract HCV during birth.
However, little is known about the transmission of HCV in comparison to HBV and HIV. Vaccination for HBV does not protect against infection with HCV.
Tuberculosis
Tuberculosis is one of the few diseases that is spread via the airborne route. Aerosolized bacteria may remain suspended in the air for long periods of time and inhaled into the lungs of a susceptible person. TB continues to be a major health burden in the twenty-first century with millions of deaths every year.
Infection may occur when inhaling particles released when someone with active TB coughs, sneezes, speaks, or sings. These can remain airborne within small droplets for several hours and susceptible individuals can still become infected.
Only patients with active TB can transmit the disease. In latent infection the bacteria remain viable in the body for many years without causing an active infection but retain the ability to activate under favorable conditions. It is not possible to predict who will develop active TB at some point.
So, dental staff may be at increased risk of exposure to TB. Because masks worn in dental offices are not considered adequate to prevent transmission of tuberculosis, it is important to identify patients at high risk.
Patients who are suspected of having tuberculosis should be referred to an appropriate physician for diagnosis and treatment before receiving dental treatment.
If emergency dental treatment is necessary for patients with active tuberculosis, they should be referred to a specialized facility with negative pressure and adequate air exchanges.
Staphylococcus aureus
S. aureus is one of the most common causes of both community-acquired and hospital-acquired infections.
The nose and mouth are the natural habitat of S. aureus, and carriage on dentures has been reported. They may transmit the organism to dentists through shedding from their noses or via their hands if infection control practices are inadequate.
Other Bacteria
A number of bacteria may be found in the mouth and throat of people who show no symptoms. Asymptomatic carriers can transmit these bacteria to susceptible people in whom infection can occur. The route of transmission is via droplet spread, which can be prevented by wearing a mask and washing or disinfecting hands.
Precautions
The routine precautions such as vaccination and cough etiquette may help prevent disease transmission in healthcare settings, standard precautions are used.
These may help to reduce the risk for infection among patients and clinicians.
Standard precautions include the use of protective attire such as gloves, masks, gowns and protective eyewear; disinfection and sterilization processes; hand hygiene; safe injection practices; and safe handling of potentially infectious materials.
In reputed dental clinics in Delhi, patients are being educated thoroughly about maintaining standard precautions from infected individuals.
Diseases that spread by the airborne route, such as chicken pox (until lesions are crusted over), TB, measles, or herpes zoster (until lesions are crusted over), require airborne precautions in addition to standard precautions.
Depending on the situation, it may be necessary to delay non-emergency dental treatment for patients with certain illnesses.
The treatment for patients with these active or incubating diseases should only be performed in a facility equipped with an airborne infection isolation room.
If no immediate treatment is needed, the patient should be asked to return when symptoms have dissipated. If immediate treatment is needed, the patient should be transferred to a facility with an airborne-infection isolation room.
Posted by- Dr Shriya