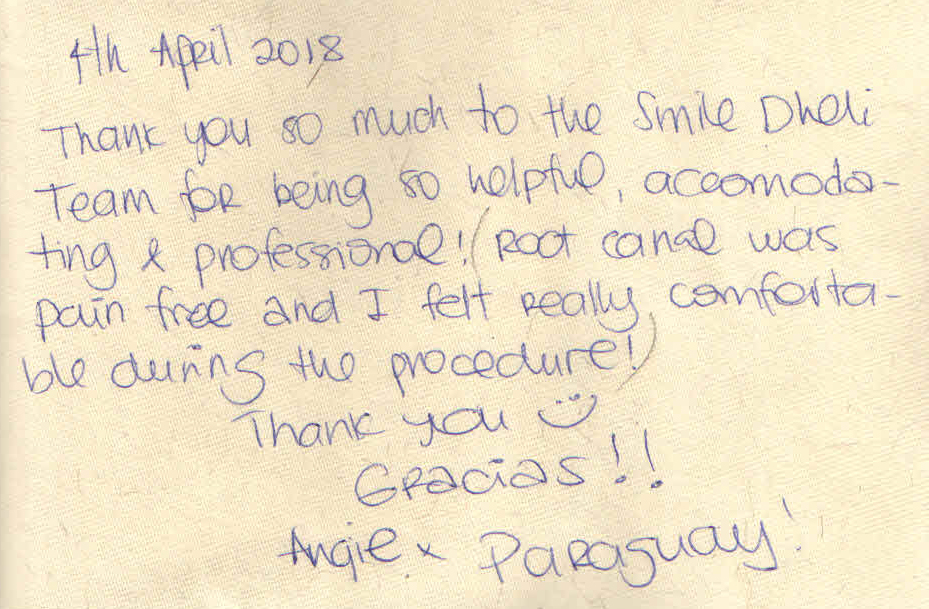Dry Socket
Dry socket (alveolar osteitis) is a painful dental condition in which there is inflammation of the jawbone that can occur after you have a permanent adult tooth extracted. The jawbone may be visible in the socket as a white area where it would normally be covered with a blood clot or healing membrane.
It involves a situation where an extraction site’s healing process is interrupted (delayed) due to the loss of the blood clot that normally occupies the empty tooth socket after tooth extraction. The socket is the hole in the bone where the tooth has been removed.
After a tooth is pulled or extracted, normally a blood clot forms in the socket at the site of tooth extraction as the first step in healing to cover and protect the underlying jaw bone and nerves underneath. This blood clot serves as a protective layer over the underlying bone and nerve endings in the empty tooth socket. The blood clot has two functions: It stops the area from bleeding and over time, stimulates bone healing by providing the foundation for the growth of new bone and for the development of soft tissue over the clot.
Sometimes that blood clot can become dislodged or dissolve a couple of days after the extraction, before the wound has healed. If the blood clot is lost or does not form, the bone is exposed which is extremely painful. As this leaves the bone and nerve exposed to air, food, fluid and anything else that enters the mouth and healing is delayed.
This can lead to infection and severe pain(aching, throbbing pain), not only in the socket(gum or jaw) but also along the nerves causing radiating pain up and down the face and pain upon drinking cold water or breathing in cold air. With this onset of pain, it is obvious that proper healing has been interrupted.
It is imperative to keep the blood clot in the socket until the bone has a chance to fill the socket and essentially heal. Without the blood clot, the socket will take longer to heal and it will be quite painful during that period of time.
Think of the blood clot as a scab on a deep cut on your skin; if the scab comes off too early, the area is exposed and can be painful, just like a dry socket.
During normal healing, the discomfort of an extraction should lessen over time. However, if the pain increases, this is an indication that healing is delayed and could possibly be due to a dry socket.
Normally, post extraction pain peaks and wanes within a 24 hour period, but dry socket pain peaks 3 to 5 days after the extraction, the level of pain actually starts to intensify and take weeks to go away unless treated by a professional.
Dry sockets are rare and occur in 5% of all tooth extractions. Studies have shown that women are more likely than men to develop a dry socket, which could be due to menstrual cycles and estrogen levels. The reason there is so much pain when the blood clot is lost is because the pain receptors in the jaw bone are completely exposed to the outside world.
The occurrence of dry socket is relatively rare, occurring in about 2% of tooth extractions. However, that percentage rises to at least 20% when it involves the surgical removal of mandibular impacted third molars (lower wisdom teeth). So in dental clinics in Delhi, oral surgeons are specially empaneled to do the removal of lower wisdom teeth. Thus proper expertise prevents this problem of dry sockets to a large extent.
Over-the-counter medications alone won’t be enough to treat dry socket pain. Your dentist or oral surgeon can provide treatments to relieve your pain and promote healing.
Average healing time is 7 to 10 days, as this is the amount of time it takes for new tissue to grow to cover the exposed socket. Once the tissue is able to cover the bone, the healing will progress normally.
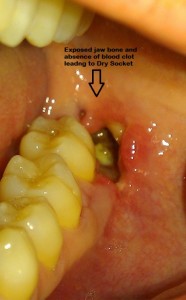
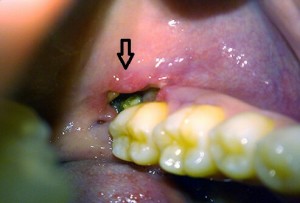
Signs and Symptoms of Dry Socket?
- Severe pain(throbbing) typically starts about two to four days after a tooth extraction
- Discomfort from the extraction site typically starts to intensify 3 to 4 days and usually runs for 4 to 8 days after the tooth was initially removed. The discomfort can be constant or intermittent (its frequency can vary).
- Partial or total loss of the blood clot at the tooth extraction site, which you’ll probably notice as an empty-looking (dry) socket.
- Visible bone in the socket instead of a blood clot
- Pain is frequently described as a dull throbbing pain. It can be moderate to severe in intensity.
- Pain may remain localized in the area of extraction site or overtime pain can radiate from the socket to your ear, eye, temple or neck on the same side of your face as the extraction
- The gum tissue around the extraction site is typically reddened and inflamed.
- Bad breath or a foul smell coming from your mouth
- Unpleasant taste in your mouth due to accumulation of food debris and bacteria in the socket.
- Swollen lymph nodes around your jaw or neck
Characteristically, these symptoms do not appear until a few days after the tooth was removed.
Risk Factors of Dry Socket?
The precise cause of dry socket remains the subject of study; several issues may be at play. Factors that can increase your risk of developing dry socket include:
- Bacterial contamination of the socket(tooth or gum infection): Current or pre-existing active infection that is present in the mouth or around the tooth to be extracted prior to a dental extraction such as periodontal disease (or periodontist) can prevent proper formation of a blood clot.
- Smoking and tobacco use- Smoking is a risk factor for developing dry socket due to nicotine found in cigarettes. Chemicals in cigarettes or other forms of tobacco may prevent or slow healing and contaminate the wound site. Exposure to nicotine reduces the blood supply in the mouth. As a result, the blood clot may fail to form at the site of a recent tooth extraction. The act of sucking on a cigarette may physically prematurely dislodge the clot or prevent the proper formation of the blood clot at the extraction site.
- Sucking through a straw, aggressive rinsing, spitting, or dragging on a cigarette after having a tooth extracted causes dislodgement and loss of the blood clot.
- Age- Density of bone decreases with age. Dense jawbone, or poor blood supply are factors that prevent blood clot formation. A dense jawbone increases the risk of a traumatic extraction and less blood supply decreases the chances of blood clot formation and timely healing. Additionally, relatively older people generally have a comparatively lower capacity of healing.
- Hormone levels or oral contraceptives- Women have been found to develop a dry socket more so than men due to hormonal factors. High estrogen levels from the use of oral contraceptives or normal hormonal changes during a woman’s cycle may disrupt normal healing processes and increase the risk of dry socket.
- Severe bone and tissue trauma (greater than the usual trauma) at the surgical site due to a difficult extraction. For example, extraction of impacted third molars (wisdom teeth) can be traumatic as some surrounding gum tissue and jawbone may need to be removed or may be adversely affected during surgery. Although the extraction is necessary, the resulting trauma can increase the chances of dry socket.
- Very small fragments of roots or bone remaining in the wound after surgery.
- Improper at-home care- A high bacteria count in the region of extraction site (existing either before or after the extraction) due to poor oral hygiene can cause the breakdown of the clot. Proper at-home care after a tooth extraction helps promote healing and prevent damage to the wound. Failure to follow guidelines may increase the risk of dry socket.
- Having dry socket in the past- If you’ve had dry socket in the past, you’re more likely to develop it after another extraction.
- Use of corticosteroids- These types of medications, such as prednisone, may increase your risk of dry socket.
What is the treatment of the dry socket?
In dental clinics in India and especially in reputed dental clinics in Delhi , a very systematic approach is followed for diagnosis and evaluation of dry socket- Dentist will first need to establish that it is likely that you do indeed have a dry socket.
They will ask you about the nature of your symptoms and inspect your wound. They’ll also want to know about the timing of the events you’ve experienced.
Drawing on their expertise they can determine what the most likely cause of your problem is and how it should be treated (just because you personally think you have a dry socket doesn’t mean that you do).
Treatment usually involves symptomatic support while the socket heals. Initially, the dentist will gently flush your extraction site to clear the socket, removing or washing away any food debris from the hole that might inhibit the healing process. As ineffectual cleansing of debris from the tooth socket aid or possibly promote formation of a secondary bacterial infection.
Next, an analgesic medicated dressing is placed within the socket to cover or insulate the exposed bone and to promote healing. This usually provides immediate relief from the pain during the extended healing process as well as mimic what the blood clot would have done. Since this dressing needs to be replaced every few days, dentists in dental clinics in Delhi provide a regime for these patients to come every 2 or 3 days regularly, until the socket starts to heal and the pain lessens. The dressing is often coated with “dry socket paste,” which is made up of ingredients with pain-relieving properties, including eugenol (clove oil).
Packing the socket with bone graft material or surgical foam may also be one of the treatment option but it is a long term solution, albeit more expensive. Usually in the dental clinics in india, the option of putting dressing is adopted.
Additionally, medications can be prescribed to prevent the socket from becoming infected (pus) and to manage the pain and to ease the discomfort. Always keep in mind that pain pills are meant to be swallowed. Placing one on, or in the region of, your dry socket will not be effective and will result in extraction site irritation.
To care for the dry socket at home, your dentist may recommend that you rinse with warm salt water or a special mouthwash every day.
Is it possible to prevent a dry socket?
The prevention of developing a dry socket may be influenced by the methods used by the dentist or surgeon performing the tooth extraction.
Such preventive methods include (1) placement of a packing at surgery with or without antibiotic and/or (2) placement of sutures to protect the blood clot. These details can be discussed with the dentist or surgeon prior to the procedure to determine if these preventive methods would be recommended.
After extraction, there are a few day-to-day activities that should be avoided: smoking, drinking with a straw, drinking carbonated beverages (soda, beer, sparkling water etc.) and vigorous spitting or rinsing. It is important to follow any special instructions given by the dentist or surgeon in caring for the extraction site at home.
The dentist in Delhi, take a thorough history of the patient. Because smoking is a big risk factor for dry socket, avoid cigarettes, cigars and any other tobacco products. As difficult as it may be, if you are a smoker you can lower your chances of getting a dry socket by not smoking on the day of surgery, and then for as many days afterwards as is possible.
Also, check with your dentist about other medications you are taking that can interfere with normal blood clotting.
After your surgery, avoid drinking through a straw and spitting for the first few days. Also don’t rinse your mouth more than your dentist recommends. If you do rinse, do so gently. Remember to visit your dentist for follow-up visits.
Lastly, recent studies have shown that the incidence of dry socket with women is significantly decreased when tooth extractions are performed during their menstrual period (menses). When teeth extractions can be electively planned, the recommendation is to perform this procedure during the menstrual period. In this way, the risk of dry socket due to cycle-related hormonal changes can be eliminated. If you take birth control pills, ask your dentist about performing the extraction on a day when you are getting the lowest dose of estrogen because the hormone can affect the ability of the blood to clot.
Both in dental clinics in Delhi and dental clinics in India, the proper post-extraction protocol is advised by the dentists. Adhering to this protocol and following the dentist’s directions always helps with dry socket prevention, no matter what your underlying baseline risk might be.
Posted By – Dr. Shriya